Cataclysm
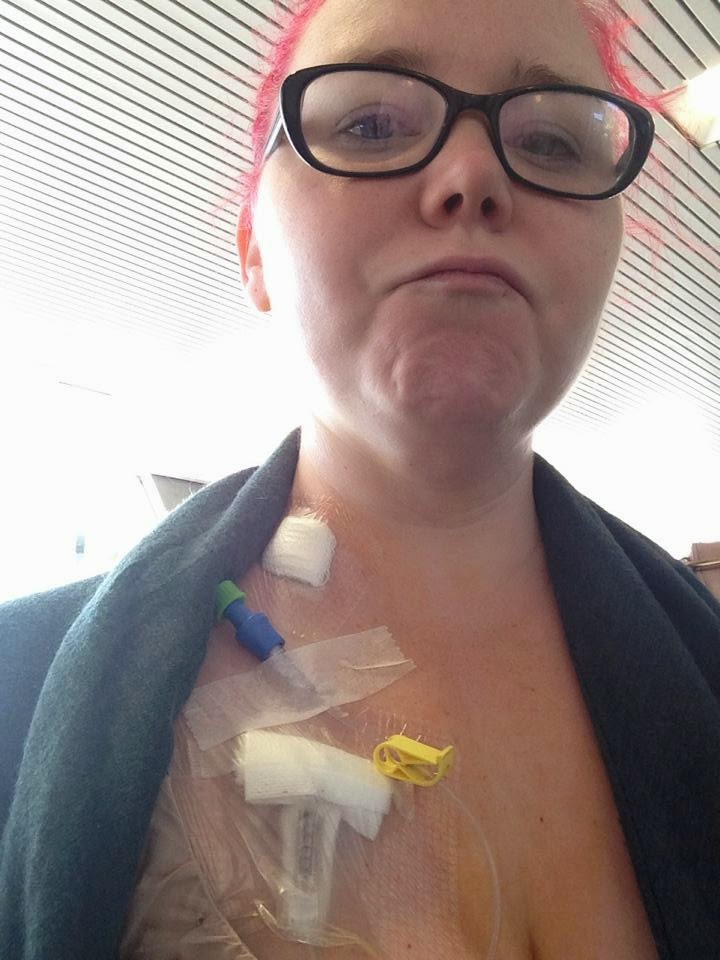
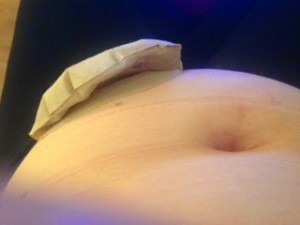
I have had a central line for four and a half years. We placed a PICC line in early 2014 to facilitate vascular access in an emergency, to administer rescue meds at home during an anaphylactic event, and to allow me to use IV fluids at home to stabilize my blood pressure.
Shortly after I had my line placed, I was hospitalized for a five day long episode of protracted anaphylaxis. Because I had pretty much already tried every oral medication that could help manage my symptoms, trying IV medications was the obvious next step. I went home from the hospital with a prescription for IV Benadryl.
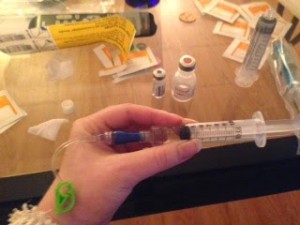
Speed matters a lot in management of mast cell disease. There is a tiny window of time during which immediate medication can stave off continued reaction or anaphylaxis. I learned how to dilute and push IV Benadryl during mast cell crisis.
Using IV meds was really nerve wracking at first, much more than I expected it to be. I’m an infectious diseases microbiologist by training and used to develop diagnostics for blood stream infections. I don’t think I can overstate how scared I was of getting sepsis. Every time I touched my line to flush or give meds, my hands shook and my heart pounded. But this was tempered by an obvious benefit: use of IV Benadryl as soon as a reaction started often prevented the need for epinephrine.
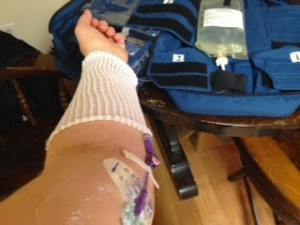
My health fluctuated over time. Eventually, I started using IV Benadryl as a baseline medication to manage daily reactions. It allowed me to exercise. It allowed me to eat. It allowed me to travel. It allowed me to work. IV Benadryl restored a much improved quality of life. I have used it ever since.
IV Benadryl is an old medication. It is off patent, cheap to produce, and made by multiple manufacturers licensed in the US. Overwhelmingly, it is used to manage anaphylaxis. Regular use as maintenance for patients was unheard of before the mast cell community began using it to manage reactions. Home use of IV Benadryl both for maintenance and for rescue – that is, to manage regular daily symptoms as well as to be lifesaving in the event of anaphylaxis – has become more popular in the mast cell community in recent years. I think I’m probably partly to blame for this – I have openly talked about how much it has helped me. I probably know a hundred mast cell patients who use it regularly.
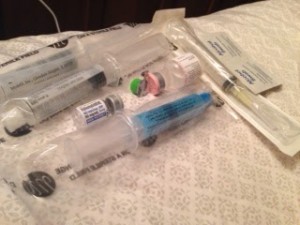
In mid September, I got a call from my IV pharmacy. They were calling to tell me that vials of IV Benadryl were unable and they were going to dispense IV Benadryl in prefilled syringes. Fine. I didn’t care what package it was in. But I knew multiple organizations made this medication and I found it strange that vials from all of them would be unavailable at the same time. It was odd. But it was also true. Every manufacturer was reporting that it would be several weeks to months before the vials would be again be available.
A week later, my IV pharmacy called to let me know that the prefilled syringes were no longer available either. I found out on a Friday afternoon that come Tuesday, I would be out of medication. No one could get it. All distributors were out. I called over fifty pharmacies in Massachusetts trying to find some. I talked to the FDA. I talked to the manufacturers. I talked to hospitals nearby.
Despite being labeled a “critical backorder”, this phenomenon was something else entirely. It wasn’t “I can’t get enough of it.” It was “There is no IV Benadryl available anywhere in the US.” EMS is out. Hospitals are out. And every pharmacy everywhere is out or dangerously close. With only a few days warning, mast cell patients found themselves unable to get medication that literally kept them alive.
It is not overstating things to say that IV Benadryl is necessary to sustain life in a number of mast cell patients. I am one of them. Many people need it to maintain an airway. Others, like me, need it to recover blood pressure during anaphylactic shock. A lot of patients were only able to live outside of a hospital safely because they had access to this medication. The danger posed to these people is enormous. This is especially true because in an emergency, you can call 911 and have them take you to the hospital but they don’t even have the medication to treat you. This means that unless patients already have some, in a crisis, it is impossible to get more from literally anywhere. If you need this medication to survive, you are in real peril.
Compounding the issue is that IV Benadryl is the only potent H1 antihistamine available in IV form in the US. There are no alternatives for IV H1 antihistamines. It is IV Benadryl or IV nothing. It is also not used much outside of the US so getting it from abroad isn’t really an option.
Mast cell patients have been encouraged to use epinephrine as early as possible without IV Benadryl to potentially stave off a reaction. So we can all just use epipens anytime we react badly, right? Just kidding. Epipens are also on critical backorder. Okay, let’s use IV fluids to recover blood pressure during anaphylaxis and severe allergic symptoms. Haha, no. IV fluids are also on backorder. One of the safe narcotics for mast cell disease is no longer available. Certain benzodiazepines are no longer available. And we have no idea whether or not these medications will be available in the future.
The stress of this situation is paramount. I have patients getting trached to allow them to be hooked up to a ventilator. I have patients who can’t stand up without reacting or passing out. I have patients who are using epi multiple times a week. And I have patients who are scared to use their epipens so they gamble that they can control their reactions with something else. The single greatest risk factor for fatal anaphylaxis is delay in the administration of epinephrine. “Saving” epipens is dangerous.
Those of us who have won some stability through this medication are terrified of going back. I am terrified of going back. It’s already starting. After several months of debilitating symptoms and repeat anaphylaxis, I have been preparing to return to work in November. I love my job. I love my coworkers. I love my company. I can’t safely return to work until I have a guaranteed supply of IV Benadryl. And as of now, that could take months.
I am angry over this situation in a way that borders on holy fury. Mast cell disease is hard on its best day. It doesn’t need to be made even harder. Total loss of access to rescue meds is life threatening for many of us. In a country known for its premier healthcare, essential medications are completely unavailable. Mast cell patients were not even notified of an impending backorder to allow us to identify a source and stockpile. We were ignored entirely. This is the end result.
This is a dark time for our community. It is a time for fear and anxiety. It is a time of uncertainty. It won’t last forever. But that is cold comfort when you are terrified.
It is also a time to stand up and fight. It is a time to be visible. It is a time to be loud. It is a time to shame these organizations for letting this happen to us. Because if I have to suffer, I will damn well make them watch.
I know a lot of us are struggling. Be careful with yourself. Don’t take risks. Wait it out.
Take care of yourselves. Remember: it won’t always be like this. You don’t have to beat it. You just have to outlast it.